

Celiac disease is very similar to a food allergy, in that it triggers immune system activity in response to certain foods being eaten. However, celiac disease is a unique condition that specifically damages the lining of the small bowel, or small intestine. The primary trigger is consumption of gluten, which is a protein molecule present in food products made from wheat and other grains, such as barley and rye. While there is no “cure” for celiac disease, Bothell’s Dr. Nicole Anderson works with patients to get a diagnosis that is as minimally disruptive as possible and develop a plan to manage symptoms.
For many years, doctors practicing traditional medicine have relied on a biopsy of the GI tract for a definitive celiac disease diagnosis. Many patients who suspect they have the condition seek out testing because of the symptoms, the most common of which are gastrointestinal issues—such as diarrhea, bloating, abdominal pain, and gas—after eating food containing gluten proteins. Symptoms beyond negative impacts to digestive health include anemia, osteoporosis, and chronic fatigue.
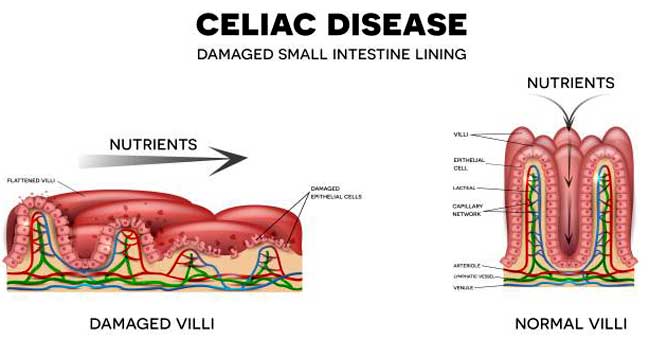
A GI biopsy is an invasive procedure that involves inserting a long endoscope through the mouth and moving it down until it can allow for a sample to be taken from the small intestine. Doctors often instruct a patient to eat significant amounts of gluten-containing foods for weeks prior to this procedure, which can dramatically worsen their symptoms. While this allows imaging of the intestinal villi for a definitive celiac disease diagnosis, it’s often simply not worth it since the intestinal damage can takes weeks or months to heal once the gluten is finally removed after a diagnosis is made.
Dr. Nicole Anderson takes a different approach, with a goal of starting the path toward a diagnosis with the least-invasive testing methods. This can be done in part by laboratory testing, as well as by removing gluten-containing foods completely from their diet for a sufficient amount of time. Patients can then observe whether their symptoms improve or not. If abdominal pain, diarrhea, fatigue, and other common problems associated with celiac disease lessen or resolve in the absence of gluten, an important first step has been made, and an invasive biopsy is not necessary.
Armed with the knowledge of what gluten or its absence does to their body, patients can pursue a more definitive celiac disease diagnosis as desired. Some of Dr. Anderson’s patients do opt to seek out a GI biopsy, while others simply remove gluten-containing products and ingredients from their diet and enjoy the physical–and often mental– improvement.
Celiac disease is a lifelong condition, but the symptoms do not have to be. Patients can quite effectively manage their symptoms through careful meal planning and improving their overall health so their whole body functions as it should.
A constant attack on the lining of the small intestine leads to nutritional deficiencies as well as chronic inflammation. This sustained immune system response can begin to impact other parts of the body as well, causing or contributing to such problems as arthritis and inflammation of the nervous and musculoskeletal systems. The longer inflammation is allowed to continue unchecked, the more damage it can do, and the more ways the body can try to “raise an alarm” that something is wrong.
When patients understand how their body reacts to gluten, they can make informed choices about their diet, their general lifestyle, and even their pursuit of diagnosis and treatment for other medical issues. Having as complete a picture as possible about health is a valuable and critical element of long-term well-being.